Diabetic eye disease refers to a group of eye conditions that occur in people living with diabetes and can affect different parts of the eye, particularly the retina—the light-sensitive layer responsible for forming clear images. Over time, elevated blood sugar levels may affect the tiny blood vessels and tissues in the eye, leading to changes in vision. These conditions can include diabetic retinopathy, diabetic macular edema, and other diabetes-related eye changes. In the early stages, there may be no noticeable symptoms, even when changes are already present. As the disease progresses, individuals may experience blurred vision, distortion, or dark spots. Regular eye examinations are important for people with diabetes so that any changes can be detected and monitored over time.


Diabetic eye disease is largely related to the effects of raised or fluctuating blood sugar levels on the small blood vessels and tissues in the eye. Persistently high blood glucose may weaken vessel walls, cause leakage of fluid or blood, and reduce the oxygen supply to the retina. Over time, the eye may respond by forming new, fragile blood vessels that are prone to bleeding. Other factors such as high blood pressure, high cholesterol, kidney disease, and smoking can further affect blood vessel health and contribute to eye complications. Duration of diabetes is also important—the longer a person has diabetes, the higher the likelihood of developing some form of diabetic eye disease.

The risk of developing diabetic eye disease increases with the duration of diabetes and the presence of other medical conditions. In the early phase, a person with diabetes may not notice any visual changes, even though tiny blood vessels in the retina are already affected. As the disease progresses, leaking vessels, swelling, and reduced oxygen supply can lead to more obvious symptoms such as blurred or fluctuating vision. In later stages, new fragile blood vessels may grow and bleed, or scar tissue may pull on the retina, leading to more serious complications. Good overall diabetes management and regular eye checks are important components of care.
Diabetes present but eye examination may appear normal or show very mild changes
Small leaks or microaneurysms in retinal vessels, often without symptoms
More widespread vessel changes, small haemorrhages, or early macular swelling
Marked vessel changes or reduced blood flow, with higher likelihood of new vessel growth
Fragile new vessels, bleeding, scar tissue, or traction on the retina, with higher risk of significant vision changes
Many people with diabetic eye disease have no symptoms in the early stages, which is why regular screening is recommended. As the condition progresses, symptoms may develop gradually or sometimes more suddenly. Vision may fluctuate from day to day, especially when blood sugar levels change. In some cases, sudden bleeding into the eye can cause a rapid drop in vision. Because other conditions can cause similar symptoms, a full eye examination is needed to determine the exact cause.



Diabetic retinopathy is the most common diabetic eye condition and occurs when long-term elevated blood sugar levels affect the tiny blood vessels that supply the retina. In the early stage (non-proliferative diabetic retinopathy), weakened vessel walls may leak fluid or small amounts of blood, and parts of the retina may receive less oxygen. When swelling involves the central macula, detailed vision can be affected. As the condition progresses to more severe forms, the retina may become increasingly deprived of oxygen, prompting the growth of new, fragile blood vessels. This later stage (proliferative diabetic retinopathy) can be associated with vitreous bleeding, scar tissue formation, or pulling on the retina, which may lead to more serious complications. Regular eye examinations and medical management of diabetes play an important role in the long-term care of diabetic retinopathy.

Diabetic macular edema occurs when fluid from leaky retinal vessels collects in the macula, the central area of the retina responsible for detailed vision. This swelling thickens the macular tissue and interferes with the fine visual tasks needed for reading, driving, and recognising faces. DME can occur at any stage of diabetic retinopathy, although it is more common as the disease progresses. In some individuals, the swelling may be mild and have little impact on vision, while in others, it can significantly blur or distort central vision. DME often requires close monitoring and may need specific treatments targeted at the leaking vessels or swelling.

Diabetes can also be associated with several other eye conditions. People with diabetes may develop cataracts earlier and more often than those without diabetes, leading to cloudy or blurred vision. Diabetes-related changes in blood vessels can also be linked with retinal vein occlusion in some patients. In certain situations, severe diabetic retinopathy with new blood vessels on the iris or drainage angle of the eye can contribute to raised eye pressure (neovascular glaucoma). Not everyone with diabetes will develop these problems, but awareness and regular eye checks help identify them when they occur.
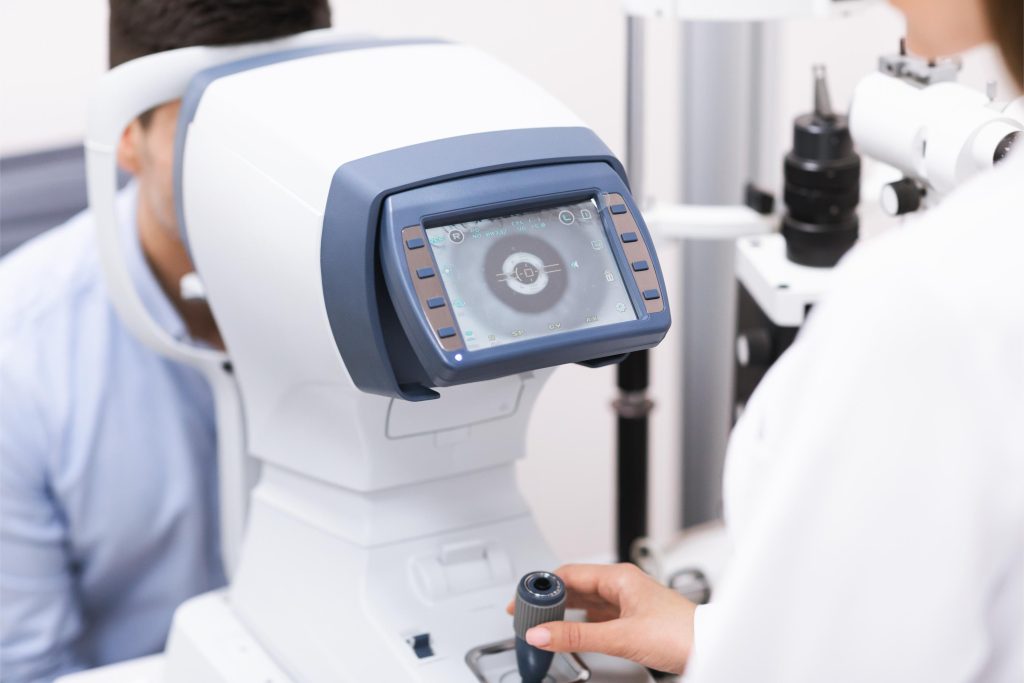
Diabetic eye tests are carried out to detect changes early, monitor progression, and guide decisions about treatment. Because diabetic eye disease can be present even when vision seems normal, these tests are recommended at regular intervals for people with diabetes. During a diabetic eye assessment, the specialist may dilate the pupils to obtain a clearer view of the retina and use imaging to document the structure of the macula and blood vessels. Functional tests can assess how well different parts of the visual field are working. Together, these tests provide a structured overview of the current eye status and how it may be changing over time.
Diabetic eye treatments focus on managing the underlying diabetes, addressing changes in the retina, and monitoring the eye over time. The choice of treatment depends on which part of the eye is affected, how far the disease has progressed, and whether there is macular swelling, bleeding, or new vessel growth. Many patients will benefit from a combination of systemic control (blood sugar, blood pressure, cholesterol) and eye-directed therapies. Eye-directed treatments may include injections, laser procedures, or surgery in selected situations. Regular follow-up allows the eye specialist to adjust the treatment plan as needed.

Every patient’s condition, lifestyle, and goals are unique — and so should their care. We take the time to listen, understand, and evaluate your needs in detail. From there, we develop a tailored treatment plan that delivers the most ideal outcomes.

For most of us, our vision is our most valued sense. Whether you are a senior, of working age, or the parent of a child who needs help, we will prioritise understanding your case and determining the most suitable treatment to improve or preserve your vision. We welcome complex cases as we care about you, your sight and your future.

We harness the power of ophthalmic technology to deliver precise diagnostics, accurate treatments, and faster recovery times. From imaging systems to minimally invasive surgical tools, our investment in technology allows us to provide safe and effective eye care.
Your safety is our highest priority. Every diagnosis and treatment we provide is evidence-based to ensure that each step of your care is not only effective but also held to a high standard of safety and quality.

For pre-surgery, we will discuss all possible treatment options and recommends the most appropriate one for every patient. For post-surgery, we provide aftercare, including follow-up consultations and treatment plans tailored to every patient to promote optimal recovery.
Wish to book a consultation or have a question? WhatsApp Us!